The Shift to Fetoscopic Repair of Myelomeningocele
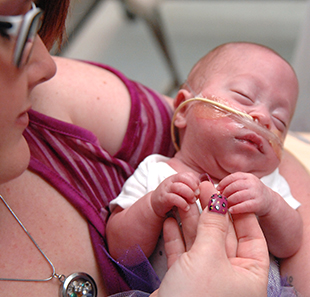
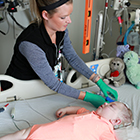
Last year, a surgical team at Cincinnati Children’s completed a study to evaluate the safety and efficacy of fetoscopic surgery for lumbar myelomeningocele. Here, pediatric neurosurgeon Charles Stevenson, MD, FAANS, FACS, FAAP, answers questions about this evolving field.
What is the rationale for prenatal repair of myelomeningocele?
Most people associate spina bifida aperta, or myelomeningocele, with lower extremity weakness and bladder dysfunction, but the fact is that its most severe form is frequently lethal. With standard postnatal repair of the defect, up to 15% of patients die within the first five years of life, usually due to hydrocephalus and brainstem dysfunction secondary to the associated Chiari II malformation. Overall mortality approaches 25% by adulthood.
The landmark Management of Myelomeningocele Study (MOMS) demonstrated the unequivocal efficacy of prenatal surgical repair in achieving its primary outcome measures for children with this condition. When compared to postnatal closure, open fetal surgery cuts the risk of hydrocephalus in half, increases a child’s chances of being able to ambulate independently, and reverses hindbrain herniation associated with Chiari II malformation in eight out of 10 patients.
What motivated you to consider fetoscopic myelomeningocele repair?
Soon after MOMS results were published in 2011, I performed the first open fetal myelomeningocele repair at Cincinnati Children’s. However, this surgery is associated with significant risks, including prematurity, placental abruption, and dehiscence of the uterus. Like other pediatric neurosurgeons, I started to think about how we could minimize the risks of this surgery while still achieving its obvious benefits. In 2016 our team established a study protocol to offer fetoscopic repair, a less invasive technique designed to minimize uterine trauma, under the auspices of the hospital’s Institutional Review Board. We initially enrolled 10 patients, and continued offering the surgery once the IRB ended in 2018.
What have you learned so far?
We have improved our surgical technique and post-operative management significantly throughout our series. Our time of surgery is comparable to that of open fetal repair, as is average gestational age at delivery. Obviously one of the biggest surgical challenges is making sure the defect closure is robust, and we have done that, with none of the babies having spinal fluid leaks upon delivery.
All children who undergo prenatal surgery at Cincinnati Children’s receive rigorous follow up at our Center for Spina Bifida Care. It is too early to draw conclusions about the efficacy of fetoscopic surgery compared to open repair, but the preliminary data is very encouraging.
What’s next?
Our team and others nationally are developing new fetoscopic techniques and technologies that will allow earlier successful intervention and further reduce surgical risks to both mother and baby. Our practice is shifting toward fetoscopic repair. When combined with a nuanced approach to long-term management, it can be a total game changer for these kids, without the inherent risks of an open surgery.