“Pancreas on a Chip” a Breakthrough in Finding Cause of Cystic Fibrosis-Related Diabetes
In a first-ever accomplishment, reported July 16 in Nature Communications, researchers in the laboratory of Anjaparavanda Naren, PhD, director of the Cystic Fibrosis Research Center, and research associate Kyu-Shik Mun, PhD, developed a chip on which they grew human pancreatic tissue from patient-derived organoids. The researchers started by isolating pancreatic ductal epithelial cells and pancreatic islets donated by surgical patients.
The two-chambered microfluidic device, just a few centimeters in size, contains biochemical solutions that generate the tissue. Ductal epithelial cells are cultured in the chip’s top chamber and pancreatic islet cells in the bottom chamber, separated by a thin layer of porous membrane that allows the two chambers to interact.
An Ideal Approach
“This is purely human tissue, from patients, not from induced pluripotent stem cells,” Naren says. “Kyu-Shik created a unique model that mimics human pancreatic structure and function.”
Studying cystic fibrosis-related diabetes (CFRD) in a milieu that replicates the human pancreas was impossible to do in vitro before. A significant number of patients with cystic fibrosis (CF) develop CFRD by young adulthood, Naren says. Although mutations in a gene known as the CFTR gene are known to cause CF, and researchers suspect it may be the culprit in the development of CFRD, the connection is unclear.
Finding the Cause of Diabetes in CF Patients
“We wanted to know, what makes these kids develop diabetes over time?” Naren asks. “So we went to the ductal site. CFTR is highly expressed in human pancreas and present only in the ducts. With the chip, we were able to inhibit CFTR function in the ducts and show that it caused a decrease in insulin secretion. As these children grow, if the ‘talk’ between the duct and the islet is impaired over time, that would lead to diabetes.” The scientists believe this confirms CFTR’s direct role in regulating insulin secretion and causing diabetes in people with CF.
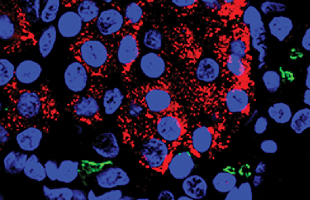 See caption below* |
Exploring Simple Solutions
Next, researchers plan to use the pancreas on a chip to test compounds that might increase the secretion of insulin. “Our hypothesis is that some kind of metabolite is being secreted from the duct to the islet that causes communication to be lost in CF. We are trying to see if metabolites, alone or in combination, can increase the secretion of insulin—and we are hoping to find a simple, inexpensive intervention for these patients,” states Naren.
*This microscopic image shows human pancreatic tissue color coded to show the presence of insulin and the gene CFTR (cystic fibrosis transmembrane conductance regulator). Researchers report in Nature Communications they used bioengineered human pancreatic tissue on a chip to determine that in addition to causing cystic fibrosis, disruption in CFTR gene expression also helps drive the dangerous complication Cystic Fibrosis-Related Diabetes.

