Innovative Care for Complex Multicystic Dysplastic Kidney Patient Results in Promising Patient Outcome
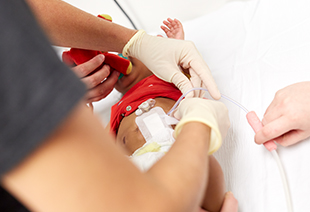
It sometimes takes a village to help a baby survive and thrive. For Baby E, diagnosed prenatally with a left multicystic dysplastic kidney (MCDK) and an absent right kidney, the collective expertise of Cincinnati Children’s fetal care team, urologists, nephrologists, transplant surgeons and many others has been lifegiving and lifechanging.
The child is one of very few babies nationally who has been anuric in utero and has survived from fetal care to transplant.
The fetal team discovered at 21 weeks’ gestation that Baby E had no kidney function. Director of Pediatric Urology Pramod Reddy, MD, notes, “My colleagues addressed the lack of fluid around the baby, which creates a buffer and allows the lungs to develop.”
Maternal-fetal specialists at University of Cincinnati Medical Center intervened by injecting saline to replace the absent amniotic fluid, i.e., amnioinfusion. This was performed a total of eight times during the remainder of her pregnancy. Reddy’s team counseled the family about the challenges of nurturing Baby E from birth to transplant, including treatment options for an undeveloped bladder.
“In most places, she wouldn’t have survived to birth or beyond,” says David K. Hooper, MD, MS, medical director of Kidney Transplantation.
As Baby E matured in utero, Foong-Yen Lim, MD, surgical director of the Cincinnati Children’s Fetal Care Center, coordinated teams of specialists at the two hospitals and provided the bridge from prenatal to postnatal care.
Pediatric nephrologist Donna Claes, MD, MS, and her dialysis team adapted equipment to put the newborn on hemodialysis postpartum to filter her blood, and aquapheresis to remove excess fluids and salt. After two weeks, Claes graduated Baby E to peritoneal dialysis, and discharged her home with her parents after four months. The team guided the family over the next two years with home peritoneal dialysis, a gastrostomy tube and medications, and maintained contact during hospitalizations, surgeries and clinic visits.
In the spring of 2021, at age 25 months, Baby E received a kidney donated by her mother.
Pediatric transplant surgeon Greg Tiao, MD, performed successful transplant kidney vascular anastomosis to Baby E’s blood vessels. Pediatric urologist Reddy joined the procedure to perform a ureterostomy, connecting Baby E’s ureter to a stoma in her abdomen. Reddy will discuss options for reconstructing the child’s urinary tract when she is 5 or 6.
Baby E’s kidney is working well, removing toxins and enabling catchup development of language, behavior and motor skills.
“She’s now speaking words,” Reddy says. “It’s so fascinating and fulfilling to see the switch flip and watch a beautiful child emerging from the haze of renal insufficiency. She’s doing fantastic.”
Baby E was the first child born without any urine production to receive a kidney transplant at Cincinnati Children’s. Since then, two more patients with challenges similar to Baby E’s have successfully received a kidney transplant at Cincinnati Children’s.
“This achievement makes us one of the most experienced centers in the world in transplanting this rare patient population,” Reddy says.

